[embedyt] https://www.youtube.com/watch?v=8WPsIyl3By0[/embedyt]
Do you ever feel tired after eating or experience a sugar drop and sudden hunger a few hours after a meal? You are not alone. I commonly see this in my patients with histamine intolerance and mast cell activation syndrome (MCAS).
It’s often overlooked yet there is a strong connection between histamine and your blood sugar. Research has shown that blood sugar imbalances can increase your histamine levels, while histamine intolerance and MCAS can contribute to insulin resistance and diabetes. Stabilizing your blood sugar is an absolutely critical aspect of improving histamine intolerance and MCAS symptoms.
In this article, I will discuss the connection between histamine and blood sugar. You will understand what blood sugar is and how it’s related to diabetes, prediabetes, and insulin resistance. You will understand everything about histamine, histamine intolerance, mast cells, and MCAS. I will explain the connection between your blood sugar, histamine intolerance, and mast cells. I will offer some natural strategies for histamine intolerance and blood sugar imbalances.
What Is Blood Sugar
Blood sugar or blood glucose is the main sugar (glucose) found in your blood. Blood glucose comes from the food you eat and caloric-drinks you consume. Your blood’s job is to carry this blood sugar around your body to your cell as the main source of energy. It does this with the help of a hormone called insulin that helps the sugar to move into your cells (1). Keeping your blood sugar at a healthy level is critical. Too high or too low blood sugar levels can present a problem.
Diabetes is a condition characterized by too high blood sugar levels. If you have type 1 diabetes, your body is unable to make insulin to deal with your blood sugar. In type 2 diabetes, your body is either not making enough insulin or doesn’t use it well. If you have prediabetes, it means that your blood sugar levels are too high but not high enough to have a diabetes diagnosis. If you have insulin resistance, it means that your body is unable to use insulin effectively. Insulin resistance is the precursor of diabetes. Insulin resistance and prediabetes are serious risk factors for developing diabetes (2).

Hypoglycemia, on the other hand, is a condition caused by low blood sugar. It’s characterized by hunger, shakiness, anxiety, sweating, pale skin, irregular heartbeat, tiredness, dizziness, and crankiness. Blood sugar drops and experiencing hypoglycemic episodes are common among people with diabetes. However, people without diabetes may experience it as well. You may experience reactive hypoglycemia a few hours after eating a meal or fasting hypoglycemia as a result of a medication or health condition. Even if you don’t have hypoglycemia, diabetes, or prediabetes, you may experience blood sugar changes that are problems due to your diet, lifestyle, and medications you take (3). These blood sugar changes may also affect your histamine levels.
What Is Histamine Intolerance and MCAS
Histamine is a chemical that is responsible for a variety of functions in your body. It helps to get rid of allergens as part of your immune response. It communicates with your brain and triggers stomach acid release to aid digestion. In a healthy body, your body releases enzymes (diamine oxidase or DAO enzymes) to break down any histamine build-up, however, if you have too much histamine due to dietary, lifestyle, environmental, and other factors, your body won’t be able to keep up and remove all the histamine. Histamine intolerance means that you have too much histamine which affects your entire body, including your gut, brain, lungs, cardiovascular system, and hormonal health. Histamine intolerance can cause a variety of symptoms and health issues hormonal issues, headaches, skin problems, digestive issues, sleep disturbances, anxiety, fast heart rate, seasonal allergies, and more (4).
When we talk about histamine and histamine intolerance, we must also take a moment to understand mast cell activation syndrome (MCAS). Your mast cells are white blood cells found in tissues throughout your body, including your skin, digestive tracts, urinary tract, respiratory tract, reproductive organs, and surrounding nerve. They are sometimes found in your blood as well due to certain infections and diseases that they may attempt to repair once the health danger is gone. Your mast cells play an important role in your immune system. They store inflammatory mediators, including histamine inside granules. When you experience an allergic reaction, your mast cells will cause an allergic response that will trigger the release of histamine and other chemicals.
MCAS is a complex health issue that may develop due to a variety of triggers, including mold, chemicals, toxins, heavy metals, allergens, medications, infections, viruses, food, and alcohol. MCAS affects a variety of systems across your body and can lead to a range of symptoms, including rashes, hives, itching, heart palpitations, low blood pressure, headaches, anxiety, fatigue, digestion issues, dizziness, weakness, and weight changes. Many of these symptoms overlap with histamine intolerance (5, 6, 7, 8).
The Histamine and Blood Sugar Connection
As you might have noticed, certain symptoms of histamine intolerance, including rapid heart rate, anxiety, fatigue, and sleep issues overlap. Histamine and blood sugar are closely connected. Blood sugar fluctuations can affect your entire body and they certainly affect your histamine levels. Histamine intolerance and MCAS may also contribute to the development of prediabetes and diabetes.
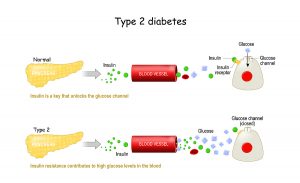
Histamine and DiabetesDiabetes is a metabolic disease. It is characterized by increased blood sugar caused by insulin resistance, the destruction of pancreatic beta cells, or the mixture of the two. Your diet, lifestyle, and various health factors can increase your risk of diabetes or directly impact diabetes. Histamine intolerance is one of these factors that may contribute to diabetes.
Research studies from the past four decades have shown the connection between histamine, blood sugar, and diabetes (9). A 1989 study published in Metabolism has found elevated histamine in those with diabetes (10). A 1990 study published in Metabolism and Cell Profeliation has found lower levels of histamine-degrading DAO enzymes in diabetic rats (11).
According to a 2010 study published in the American Journal of Pathology, histamine receptors (H1 and H2) may influence the regulation of blood sugar and lipid metabolism (12). A 2011 study published in Endocrinology has found that manipulating the H3 histamine receptor reduces blood sugar levels in diabetic mice (13). Furthermore, a 2012 study published in the ACS Medicinal Chemistry Letters and a 2018 study published in Pharmacological Research both found that targeting and inhibiting the H4 histamine receptor may be helpful for the treatment of diabetes and diabetic neuropathy (14, 15). Histamine intolerance may also increase the permeability of your blood vessels that can influence the symptoms and progression of diabetes. Clearly, the role of histamine intolerance should not be overlooked in the treatment of diabetes and vice-versa.
Mast Cell Activation and Diabetes
It is not only histamine intolerance, but mast cell activation syndrome (MCAS) can also contribute to diabetes and its symptoms. Mast cells are implicated in metabolic diseases, inflammation, and immune system issues. According to a 2016 study published in the Polish Journal of Pathology, mast cells should be taken into consideration during diabetes treatment (16).
According to a 2010 study published in the British Journal of Pharmacology, advanced glycation end products (AGEs) accumulated in people with diabetes, cardiovascular disease, cancer, and neurodegenerative disease, can activate mast cells and lead to histamine release (17). On the other hand, a 2012 study published in HHS Public Access has found that mast-cell stabilizer medications and antihistamines may be beneficial for reducing complications in those with diabetes (18).
It’s clear that there is a connection between diabetes, histamine, and mast cells. But what if you don’t have diabetes, but struggling with blood sugar fluctuations, insulin resistance, as well as, histamine intolerance or MCAS? Balancing your blood sugar is still a key step to your recovery and well-being.
Histamine Intolerance and Insulin Resistance
While there is a lot of research on the connection between histamine, mast cells, and blood glucose in those with diabetes, there isn’t any research on the connection in those without diabetes. A lot of people experience low, high, or unstable blood sugar, insulin resistance, or prediabetes without having full-blown diabetes.
In my practice, I see a lot of patients who experience blood sugar fluctuation before showing symptoms of insulin resistance or prediabetes. I also see a lot of patients with histamine intolerance and blood sugar fluctuations. A lot of people with histamine intolerance have low blood sugar and need to eat many small meals throughout the day. I also noticed that balancing your blood sugar can help to reduce or relieve symptoms of histamine intolerance.
Frequent blood sugar fluctuations can put enormous stress on your body, which can trigger histamine release and contribute to histamine intolerance and consequent symptoms. The good news is that with appropriate dietary strategies, lifestyle changes, and supplementation, you can balance your blood sugar and free yourself from symptoms of histamine intolerance.
Natural Solutions for Blood Sugar Imbalance and Histamine Intolerance
If you are dealing with blood sugar imbalance, histamine intolerance, or MCAS, there are a few natural strategies you can try. Here is what I recommend:
Measure Your Blood Sugar
I recommend that you try using a glucometer to test the stability of your blood sugar. This is an easy and inexpensive method to measure your blood sugar to support your treatment plan and see your progress. Based on your results, you can adjust your diet and lifestyle to support healthy blood sugar levels. If you are uncertain how to do this, a functional medicine doctor, like myself, can help you with a personalized nutrition plan to support your health.
Try Blood Sugar Regulating Herbs
While your diet and lifestyle are critical for stabilizing blood sugar levels, there are a variety of herbs that can help to support your blood sugar levels naturally. Some herbs I recommend include aloe vera, Nopales cactus, bitter melon, milk thistle, fenugreek, and ginger (19, 20, 21, 22, 23).
Be Smart with Sugar
If you have blood sugar issues or any health issues (or simply want to avoid health issues!), removing refined sugar and sugary processed foods is critical. You may notice though that The 4-Phase Histamine Reset Plan is not a no-sugar plan and I allow fruits and many scratchy vegetables, such as carrots or beets. If you have blood sugar issues or you find that these higher glycemic index fruits and vegetables are causing blood sugar imbalances and symptoms, you may want to reduce or remove higher glycemic index foods and choose low glycemic index fruits, such as berries and vegetables, such as cucumber or celery instead. For sweeteners, use stevia or monk fruit, which are natural and healthy options that do not disrupt your blood sugar levels.
Follow an Anti-Inflammatory and Low-Histamine Diet
Following an anti-inflammatory, antioxidant-rich, and nutrient-dense diet is important for your health. Reducing histamine may help to decrease histamine-related issues.
Remove inflammatory foods, including refined sugar, refined oils, canned and processed meat, artificial ingredients, junk food, and highly processed foods. Avoid high-histamine foods, such as fermented food (e.g., sauerkraut, kimchi, fermented vegetables, kombucha, etc.), aged food (e.g., aged cheese, processed meat, canned fish, etc.), over-ripe fruits and vegetables, leftovers, and foods that are naturally high in histamine (e.g., avocadoes, eggplant, spinach, dried fruits, etc.). Avoid foods that may trigger histamine releases, such as tomatoes, most citrus, bananas, most nuts, and dairy. Avoid foods that may block the DAO enzyme, including black tea, green tea, alcohol, and energy drinks.
Eat a nutrient-dense, anti-inflammatory, and low-histamine diet rich in greens, vegetables, herbs, spices, fruits, healthy fats, and organic meat. Low-histamine foods include most fresh leafy greens and vegetables, non-citrus fruits, such as apples, pear, papaya, and grapes, fresh grass-fed meat, pasture-raised poultry and eggs, and wild-caught fish, olives, extra-virgin olive oil, ghee, coconut oil, leafy herbs, and herbal tea. My book, The 4-Phase Histamine Reset Plan includes an extensive list of foods that you can eat and should avoid on a low-histamine diet.
If you are new to a low-histamine diet, remember to have fun experimenting with new foods and recipes. I promise low-histamine meals can be delicious. I recommend all the low-histamine recipes in The 4-Phase Histamine Reset Plan and my new recipe book, Fifty One Low Histamine Air Fryer Recipes. They are all simple, easy to make, low-histamine, gluten-free, Paleo-friendly, and super healthy. Not to mention how delicious they are — your family will love them too.
Reduce Your Histamine Bucket
If you are dealing with symptoms of histamine intolerance, reducing high-histamine foods is not enough. High stress, poor sleep, not moving your body, and high toxin exposure may add to your histamine load. Improving these areas of your lifestyle may help to reduce your histamine bucket and lower the risk of histamine-related issues.
Remove Toxins
Toxin overload can increase inflammation, histamine intolerance, and related symptoms. It’s critical that you lower your daily exposure to environmental toxins. Choose purified water over tap water. Use a high-quality air filtration system for better indoor air. Choose natural, organic, and homemade cleaning, personal hygiene, and beauty products instead of conventional brands loaded with chemicals. Choose glass, bamboo, wood, organic cotton, silicon, and other natural alternatives instead of plastic. Avoid BPA plastic completely. Choose organic food whenever possible and avoid overly processed packaged foods. If you must buy non-organic produce, follow the Dirty Dozen, Clean 15 list, and always wash and peel non-organic vegetables and fruits.
Reduce Your Stress Levels
Chronic stress may increase mast cell activation and histamine intolerance and histamine-related symptoms. To decrease your stress levels, I recommend practicing breathwork, meditation, positive affirmation, journaling, yoga, grounding, and time in nature for stress and anxiety reduction. Taking an Epsom salt bath is another great way to relax your muscles, calm your mind, and detoxify your body.
Get Enough Sleep Sleep
Inadequate and poor sleep may also increase stress. It may also trigger histamine and histamine-related issues. Improving your sleep is absolutely essential for your health. Your goal should be to sleep at least 7 to 9 hours a night. Lower your stress levels throughout the day but especially in the evening time to support sleep. Take a bath, read a good book, listen to some music, journal, try coloring, and spend time with your family. Avoid sugar, alcohol, and heavy food in the evening. Sleep on a supportive mattress with comfortable and supportive pillows and blankets, and quality, organic cotton sheets.
Move Your Body
A lack of movement may also increase the risk of histamine intolerance and related symptoms. Moving your body is a great way to reduce stress, improve detoxification, and improve your overall health. Move your body throughout the day. Stretch regularly. Take a stroll in the nearby park. Find creative ways to incorporate movement, such as an impromptu dance session, learning a new TikTok dance, playing with your kids or pets, taking the stairs, trying a treadmill desk, or practicing chair yoga. Exercise at least 20 to 30 minutes five days a week and move your body regularly. I recommend getting 10 to 15K steps in a day if you can. Add resistance and strength training to your routine.
Take HistoRelief
To support your body and reduce symptoms of histamine intolerance or MCAS, I recommend HistoRelief. This mast stabilizing supplement is a synergistic blend of nutrients including Tinofend®, quercetin, nettle leaf, vitamin C, and bicarbonate salts, that provides natural support to balance your immune response, inflammation reduction, and histamine release.
Support Your Gut
Your gut health affects your entire body. Gut flora imbalance can trigger both histamine intolerance and related symptoms. Gut microbiome inbalance may also increase blood sugar imbalances. Supporting your gut health is critical for your recovery. Along with a gut-friendly, low-histamine, anti-inflammatory diet, I recommend that you take a high-quality probiotics supplement, to support your gut microbiome balance.
Final Thoughts
There is a strong connection between histamine and your blood sugar. Blood sugar imbalance can increase your histamine levels, while histamine intolerance and MCAS can contribute to insulin resistance and diabetes. Stabilizing your blood sugar is essential for improving histamine intolerance and MCAS symptoms. Follow my tips for histamine intolerance, MCAS, and blood sugar imbalance to reduce your symptoms, increase your energy, and improve your health and well-being.
If you are dealing with symptoms of histamine intolerance and interstitial cystitis, I invite you to schedule a consultation with us. We can help identify the root cause of your condition and recommend a personalized treatment plan to repair your body and regain your health and well-being. Schedule your consultation here. I also recommend that you check out my Histamine Online Program.
Sources:
1. Blood sugar. MedlinePlus. Link Here
2. Diabetes. MedlinePlus. Link Here
3. Hypoglycemia. WebMd. Link Here
4.Maintz L, Novak N, Histamine and histamine intolerance, The American Journal of Clinical Nutrition, Volume 85, Issue 5, May 2007, Pages 1185–1196. Link Here
5. Afrin LB, Self S, Menk J, Lazarchick J. Characterization of Mast Cell Activation Syndrome. Am J Med Sci. 2017;353(3):207-215. Link Here
6. Frieri M, Patel R, Celestin J. Mast cell activation syndrome: a review. Curr Allergy Asthma Rep. 2013;13(1):27-32. Link Here
7. Akin C, Valent P, Metcalfe DD. Mast cell activation syndrome: Proposed diagnostic criteria. J Allergy Clin Immunol. 2010 Dec;126(6):1099-104.e4. doi: 10.1016/j.jaci.2010.08.035. Epub 2010 Oct 28. PMID: 21035176
8. Petra AI, Panagiotidou S, Stewart JM, Conti P, Theoharides TC. Spectrum of mast cell activation disorders. Expert Rev Clin Immunol. 2014;10(6):729-739. Link Here
9. Pini A, Obara I, Battell E, Chazot PL, Rosa AC. Histamine in diabetes: Is it time to reconsider? Pharmacol Res. 2016 Sep;111:316-324. doi: 10.1016/j.phrs.2016.06.021. Epub 2016 Jun 22. PMID: 27343700
10. Gill DS, Barradas MA, Fonseca VA, Dandona P. Plasma histamine concentrations are elevated in patients with diabetes mellitus and peripheral vascular disease. Metabolism. 1989 Mar;38(3):243-7. doi: 10.1016/0026-0495(89)90082-6. PMID: 2918844
11. Fogel, W.A., Chmielecki, C., Grałek, M. et al. Histamine metabolism in diabetic rats. Agents and Actions 30, 243–246 (1990). Link Here
12. Wang KY, Tanimoto A, Yamada S, Guo X, Ding Y, Watanabe T, Watanabe T, Kohno K, Hirano K, Tsukada H, Sasaguri Y. Histamine regulation in glucose and lipid metabolism via histamine receptors: model for nonalcoholic steatohepatitis in mice. Am J Pathol. 2010 Aug;177(2):713-23. doi: 10.2353/ajpath.2010.091198. Epub 2010 Jun 21. PMID: 20566747
13. Henry MB, Zheng S, Duan C, Patel B, Vassileva G, Sondey C, Lachowicz J, Hwa JJ. Antidiabetic properties of the histamine H3 receptor protean agonist proxyfan. Endocrinology. 2011 Mar;152(3):828-35. doi: 10.1210/en.2010-0757. Epub 2011 Jan 14. PMID: 21239440
43. Ashwin U. Rao, Ning Shao, Robert G. Aslanian, Tin-Yau Chan, Sylvia J. Degrado, Li Wang, Brian McKittrick, Mary Senior, Robert E. West, Shirley M. Williams, Ren-Long Wu, Joyce Hwa, Bhuneshwari Patel, Shuqin Zheng, Christopher Sondey, and Anandan Palani. Discovery of a Potent Thiadiazole Class of Histamine H3 Receptor Antagonist for the Treatment of Diabetes. ACS Medicinal Chemistry Letters 2012 3 (3), 198-202. Link Here
15. Pini A. Histamine H4 receptor antagonism prevents the progression of diabetic nephropathy in male DBA2/J mice. Pharmacological Research. Volume 128, February 2018, Pages 18-28. Link Here
16. Kempuraj D, Caraffa A, Ronconi G, Lessiani G, Conti P. Are mast cells important in diabetes? Pol J Pathol. 2016;67(3):199-206. doi: 10.5114/pjp.2016.63770. PMID: 28155967
17. Sick E, Brehin S, André P, Coupin G, Landry Y, Takeda K, Gies JP. Advanced glycation end products (AGEs) activate mast cells. Br J Pharmacol. 2010 Sep;161(2):442-55. doi: 10.1111/j.1476-5381.2010.00905.x. PMID: 20735427
18. Wang J, Shi GP. Mast cell stabilization: novel medication for obesity and diabetes. Diabetes Metab Res Rev. 2011 Nov;27(8):919-24. doi: 10.1002/dmrr.1272. PMID: 22069285
19. Mourad A. Beneficial effects of Aloe vera in treatment of diabetes: Comparative in vivo and in vitro studies. Bulletin of Faculty of Pharmacy, Cairo University, Volume 51, Issue 1, June 2013, Pages 7-11. Link Here
20. Ghorbani A. Best herbs for managing diabetes: a review of clinical studies. Braz. J. Pharm. Sci. vol.49 no.3 São Paulo July/Sept. 2013. Link Here
21. Voroneanu L, Nistor I, Dumea R, Apetrii M, Covic A. Silymarin in Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. J Diabetes Res. 2016;2016:5147468. doi: 10.1155/2016/5147468. Epub 2016 Jun 1. PMID: 27340676
22. Ranade M, Mudgalkar N. A simple dietary addition of fenugreek seed leads to the reduction in blood glucose levels: A parallel group, randomized single-blind trial. Ayu. 2017 Jan-Jun;38(1-2):24-27. doi: 10.4103/ayu.AYU_209_15. PMID: 29861588
23. Daily JW. Efficacy of ginger for treating Type 2 diabetes: A systematic review and meta-analysis of randomized clinical trials. Journal of Ethnic Foods. Volume 2, Issue 1, March 2015, Pages 36-43. Link Here
You Might Also Like
5 Hashimoto’s Foods to Avoid
Diet and thyroid health go hand in hand. Foods can either fuel health or cause some serious health issues…
Brain Fog: Mold’s Surprising Impact on Cognitive Function
A Functional Medicine Approach to Brain Fog Caused by Mold Exposure Ever feel like your brain is stuck in molasses? You…
Ready to Improve Your Health?
Get Started on Your Journey to Wellness





