Histamine and Exercise Intolerance
We all know we’re “supposed to exercise.” It’s good for us, it helps control our blood pressure, our blood sugar; it helps improve our mood and combat the symptoms of anxiety and depression because it causes our body to release endorphins. So why wouldn’t you exercise is the question…
Picture this: you get on the elliptical at the gym and start pedaling. Within 3 minutes, you already feel light-headed, your fingers and toes have gone all tingly, and you’re starting to feel like you could black out at any moment. You get off the elliptical, take a few deep breaths, and take a swig of water. You decide you’re going to skip the elliptical today and go right into some of your planned weight training. You grab a pair of dumbbells, and with one in each hand, you start a set of stationary lunges. You’ve done three total so far, and you start feeling dizzy and light-headed again! At this point, you’ve worked out for 5 minutes and that’s all you have in you for today. You grab your water bottle and towel and stomp out of the gym, angry that this has happened to you every time you’ve tried to work out for the past few weeks. Sound familiar?! – you’re definitely not alone.
Exercise Intolerance and Mast Cell Activation Disorder
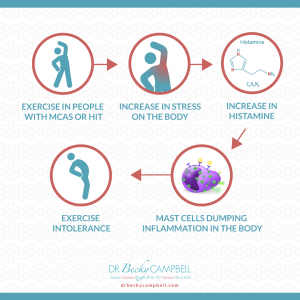
Exercise intolerance is defined as an inability or impaired ability to perform physical activity at an expected level or duration for your age and/or current fitness level. It is not necessarily a disease, but it is a symptom of a myriad of disorders. Exercise is often a problem in patients with histamine intolerance, mast cell activation disorder (MCAD), and/or mastocytosis (an accumulation of mast cells in the body). Cardiovascular exercise has been shown to increase systemic histamine levels, which can increase allergy symptoms (in animal studies) and can damage muscles, causing an inflammatory reaction to assist in the healing process (this is normal but may be excessive in patients with a histamine intolerance). Histamine is an important part of exercise because it is both created and released to prevent fatigue and improve endurance during prolonged activity. Thankfully it isn’t stored anywhere afterwards! However, exercise in patients with MCAD can be considered a stress reaction or trigger, causing mast cells to dump unnecessary inflammation into the body. Generally, mast cells can be naturally managed by including foods in your diet with ascorbic acid, quercetin, B vitamins, and omega-3 fatty acids. I also recommend HistoRelief or my Histamine Support Kit, which will provide you with a synergistic blend of nutrients that provides natural support to help balance the immune response by allowing you to naturally stabilize your mast cells, so you can slowly resume your exercise regimen with minimal symptoms. As so gracefully said by Dr. Castells, a mast cell specialist out of Boston:
“…the most important [thing] is to think about changing the lifestyle and the two most important pieces of the lifestyle are the exercise and the diet – interchangeably I mean, not one over the other.”
Postural Orthostatic Tachycardia Syndrome (POTS)
Postural Orthostatic Tachycardia Syndrome is often called the “invisible illness” because nearly every symptom is subjective. POTS is a form of dysautonomia (a dysfunction of the nerves involved in controlling involuntary bodily functions, like heart rate, blood pressure, breathing) that affects blood flow through the body. Blood flow back to the heart is decreased upon standing (orthostatic), which causes an increase in heart rate to try to correct this abnormal blood flow on the back end (tachycardia). Typically, someone has POTS if their heart rate increases by 30 beats per minute or if their heart rate exceeds 120 beats per minute within 10 minutes of standing. One of the common symptoms of POTS is dizziness upon standing, which may or may not lead to patients fainting when trying to stand up, earning POTS another nickname, the “fainting disease.” Other symptoms of POTS include:
- Headache
- Nausea
- Abdominal pain
- Chronic pain
- Heart palpitations
- Fatigue
- Shortness of breath
- Insomnia
- Brain fog
- Sweating abnormalities
- Weakness
- Bladder dysfunction
- Tremors

Diagnosis of POTS
POTS is usually diagnosed via a tilt table test in a hospital setting. Patients are strapped to the table, starting on their backs, and the table is tilted to simulate “standing up,” forcing blood to move from the upper body to the lower body. When a tilt table isn’t available, sometimes POTS is diagnosed by monitoring changes in heart rate and blood pressure when the patient is moving from lying to standing. POTS is often misdiagnosed as a anxiety or psychological disorder.
Treatment for POTS
Since symptoms of POTS are so subjective, there is no single treatment method that is going to work for everyone. Typically, there are three main treatments for POTS: diet and medication, as well as exercise, which will be discussed in the next section.
Diet
There are several recommendations pertaining to diet in order to help manage POTS symptoms.
- Increase fluid intake. POTS is caused by a rapid drop in blood pressure upon standing, so maintaining fluid volume is important to decrease these effects. Drinking at least two liters of fluids a day is recommended. There is also some evidence that drinking 2 glasses of water after a “dizzy spell” will help in alleviating symptoms.
- Increase salt intake. The amount of sodium in the body can be correlated to the amount of blood circulating. More salt means more volume, which would mean less orthostatic symptoms upon standing.
- Eat smaller meals. When you eat a large meal, more of your blood volume is going to move to your digestive symptom in order to help digest the meal you just ate. Eating smaller meals means your body won’t have to allocate as much blood to the lower half of your body, which will decrease the intensity of an orthostatic response upon standing.
- Avoid alcohol! Not only does alcohol cause an increase in histamines and a decrease in the enzyme used to break down histamine, causing a histamine response, but it also will constrict your blood vessels, making it harder for blood to return to the heart. It also functions as a diuretic, which will cause dehydration, which we want to avoid at all costs in someone with POTS (see #1 above!).
- Avoid foods that you know cause allergies or intolerances. GI distress and poor gut microbiomes can lead to an increase in histamine and also poor nutrient absorption and diarrhea, which can lead to dehydration.

Medication
Practitioners commonly prescribe beta blockers, like propranolol, for patients who have POTS. It works primarily by reducing heart rate and is shown to prevent heart rate from getting too high during exercise. This is not typically the course of action I recommend, but it is needed in some cases.
POTS and Exercise
People with POTS find themselves in a vicious cycle: they can’t feel better until they’re active, but they don’t have the stamina or endurance to be active! However, exercise is generally recommended for all patients diagnosed with POTS. Physical deconditioning is an important side effect of POTS and can actually worsen symptoms of low exercise tolerance in addition to difficulty maintaining an upright position. POTS patients have a decreased peak oxygen uptake compared to healthy individuals, which is a strong indicator of deconditioning. Please see Figure 2 for a graphic of this phenomenon.
POTS patients also demonstrate smaller heart chamber size and decreased heart muscle mass, likely due to decreased activity participation. Gradual graded exercise training has been proven to increase blood volume and cardiac muscle mass and heart size, which will result in overall
For example, in a study by Fu, et al., 2011, POTS patients were given 3 months of exercise training, 20-30 minutes, 3 times per week. Exercises started in a sitting position and gradually progressed to a higher intensity in a standing or upright position. Oxygen consumption (peak VO2) increased by 8% by the end of the 3 months, indicating a significant improvement in physical conditioning over the course of the study. Heart size and blood volume also increased. Half of the patients in the study improved so much that they no longer qualified as having a POTS diagnosis. However, it is important to remember that in order to maintain these effects, it is highly likely that these patients would need to continue with their exercise regimen after the 3 month study was completed for continued symptom relief and quality of life purposes.

Final Thoughts
I just want to share with you a story about Yasmina, a former MCAD sufferer who has unfortunately since passed away and used to blog at healinghistamine.com. Her mindset was perfectly aligned with mine in that temporary inflammation is a byproduct of exercise, but exercise long-term is generally anti-inflammatory. I also am pretty healthy and exercise consistently, but with an exposure to black mold a couple years ago, I was stuck in bed for months, too fatigued and dizzy to move. While Yasmina’s journey was obviously different from mine, she has several good take-away points that I would like to reiterate if you’re a POTS sufferer with exercise intolerance. Remember that “Rome wasn’t built in a day.” You can’t expect a body with too much histamine that hasn’t been exercising to all of a sudden just adapt to exercise, especially since now we know that exercise is temporarily inflammatory. Slow and steady is your mantra here. You exercise for 5 minutes one day and gradually increase from there.
Control your environment until you get to a place where you can exercise for an hour without any symptoms. YES! That means you don’t go to the yoga studio or the bootcamp class down the street. You find YouTube videos online and do yoga or cardio in your home, where you control what you’re near, what smells are there, how hot is is, what surface you’re on, etc. It sounds crazy, but exercise causes inflammation and if you’re already inflamed and irritated, you can bet it’s just going to be made worse when you’re put in a position where you don’t get your favorite place in the yoga studio by the Buddha where the light shines just right and the AC is right above you.
Lastly, be realistic with your goals and honest with yourself. Yeah, you were able to do a 60 minute SoulCycle class 2 years ago, but ever since that run in with the black mold (or whatever your triggers may be), you just haven’t been able to exercise at the same intensity. Don’t beat yourself up about it! You will get there – it’s just going to take much longer than any of us would like. You may need to take a day off in between exercise sessions when you didn’t used to before. And guess what: IT’S OKAY. You’ll be better for it in the long run. And that’s also what I’m here for: making you your best self. Please feel free to schedule a consultation with me if you can relate to any of the symptoms discussed above. Together, we’ll get you back on that spin bike!
What Can we Do About This?
#1) You must adopt a low histamine diet like the one in my book The 4-Phase Histamine Reset Plan
#2) Work on supporting the mast cells in your body with HistoRelief or the Histamine Support Kit
#3) Work with a practitioner that can help you find the underlying causes to both of these issues and create a detailed plan for YOUR body! I work with many people that deal with this and I dealt with it myself, so trust me when I tell you I feel your pain.
Click Below For this Free Resource!

* These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure or prevent any disease. If you are pregnant, nursing, taking medication, or have a medical condition, consult your physician before using this product.
References
- https://en.m.wikipedia.org/wiki/Exercise_intolerance
- https://healinghistamine.com/managing-exercise-induced-stress/
- https://myheart.net/pots-syndrome/
- https://myheart.net/pots-syndrome/diet/
- https://myheart.net/pots-syndrome/treatments/
- https://myheart.net/pots-syndrome/exercise-in-pots-syndrome/
- Fu. Q., et al. Exercise training versus propranolol in the treatment of postural orthostatic tachycardia syndrome. Hypertension. 2011 Aug;58(2):167-75.
- Fu, Q., et al. Exercise in the Postural Orthostatic Tachycardia Syndrome. Auton Neurosci. 2015 Mar;188:86-89.
- https://healinghistamine.com/histamine-intolerance-and-exercise/
You Might Also Like
Estrogen Dominance: Why It Happens (and What to Do About It)
If you’ve been told your estrogen is high, but you’re still feeling off — think heavy periods, bloating, crazy mood…
Ready to Improve Your Health?
Get Started on Your Journey to Wellness